Water for injections 2ml x 10amps
$20.00
Conclusion: Mastering Water for Injections for Optimal Results
Water for injections 2ml represents far more than a simple mixing agent. This pharmaceutical-grade product ensures the safety, sterility, and effectiveness of your peptide and hormone therapies.
Understanding the difference between sterile and Water for injections 2ml helps you choose appropriate products for your needs. Mastering proper reconstitution techniques protects your expensive peptides from damage while maintaining their full potency.
Storage protocols, contamination prevention, and accurate dosing calculations all contribute to successful outcomes. These seemingly minor details accumulate into significant differences between mediocre and exceptional results.
Source your Water for injections 2ml from reputable suppliers offering pharmaceutical-grade products with proper documentation. While slightly more expensive than questionable alternatives, legitimate WFI provides irreplaceable peace of mind.
Remember that proper technique matters as much as product quality. Even the purest water for injections becomes contaminated through careless handling or improper storage. Maintain meticulous protocols throughout every step of the reconstitution and administration process.Water for injections 2ml
Finally, track important dates vigilantly. Label both Water for injections 2ml and reconstituted peptides with opening and preparation dates. This simple habit prevents using expired solutions that compromise both safety and effectiveness.Water for injections 2ml
By mastering water for injections 2ml usage, you establish the foundation for successful peptide therapy. This knowledge protects your health, preserves your investment, and ensures you receive maximum benefits from your carefully chosen compound Water for injections 2ml
Water for Injections 2ml: The Essential Guide to Safe Peptide and HGH Reconstitution
Water for injections 2ml (WFI) represents a critical component of peptide and hormone therapy that often receives insufficient attention. Understanding this seemingly simple product ensures safe, effective administration while preventing costly mistakes that compromise your results.
This comprehensive guide reveals everything you need to know about water for injections 2ml, from understanding what makes it different from regular water to mastering proper reconstitution techniques that maximize peptide potency.
What Is Water for Injections 2ml?
Water for injections 2ml represents pharmaceutical-grade water specifically manufactured for preparing injectable medications. The 2ml volume has become the industry standard for reconstituting peptides, growth hormone, and other lyophilized compounds.
Unlike tap water or even distilled water, WFI undergoes rigorous purification processes that remove virtually all contaminants. Manufacturers use distillation, reverse osmosis, or other advanced filtration methods to achieve extraordinary purity levels.
The production process eliminates bacteria, endotoxins, pyrogens, and dissolved solids that could trigger adverse reactions when injected. Additionally, WFI contains no preservatives or additives—just pure H2O molecules meeting stringent pharmaceutical standards.
The 2ml format provides optimal reconstitution ratios for most peptide vials. This volume dilutes lyophilized compounds sufficiently for accurate dosing while maintaining reasonable concentration levels. Too little water creates overly concentrated solutions difficult to measure precisely, while excess water unnecessarily dilutes your expensive peptides.Water for injections 2ml
Pharmaceutical companies package WFI in sterile vials or ampoules that preserve purity until you’re ready to use them. Once opened, WFI maintains sterility only briefly unless it contains bacteriostatic agents.
Bacteriostatic Water vs. Sterile Water for Injections
Understanding the critical difference between these two products prevents common mistakes that waste expensive peptides or compromise safety.
Sterile Water for Injections
Standard WFI contains only purified Water for injections 2ml with no preservatives. Manufacturers sterilize it through filtration and heat treatment, ensuring zero bacterial contamination at the time of packaging.
However, sterile water remains contamination-free for only 24 hours after opening. Once you puncture the seal, bacteria from the air or your hands can enter the vial. These microorganisms multiply rapidly, making the water unsafe for injection within a day.Water for injections 2ml
This limitation makes sterile WFI impractical for most peptide users. Few people reconstitute and immediately use an entire vial of peptides. Most protocols require multiple injections over several weeks, demanding a solution that maintains sterility longer.
Bacteriostatic Water for Injections
Water for injections 2mlsolves the sterility problem by incorporating 0.9% benzyl alcohol as a preservative. This alcohol prevents bacterial growth, keeping the water safe for Water for injections 2ml up to 28 days after opening.
The bacteriostatic properties make this the preferred choice for peptide reconstitution. You can reconstitute a vial, store it properly, and draw multiple doses over weeks without contamination concerns.
However, benzyl alcohol makes Water for injections 2ml unsuitable for certain applications. Newborns and infants cannot safely receive injections containing benzyl alcohol due to toxicity risks. Additionally, some individuals experience allergic reactions to this preservative.
For peptide and hormone therapy in adults, bacteriostatic water for injections 2ml represents the optimal choice. The preserved formulation combines safety, convenience, and longevity perfectly suited to typical usage patterns.
Why the 2ml Volume Matters
The specific 2ml volume isn’t arbitrary—it reflects optimal reconstitution mathematics and practical dosing considerations.
Perfect Reconstitution Ratios
Most peptide vials contain 2mg, 5mg, or 10mg of active compound. When you add 2ml of Water for injections 2ml, you create convenient concentration ratios.
For a 5mg vial reconstituted with 2ml water, each 0.1ml (10 units on an insulin syringe) contains 250mcg of peptide. This concentration allows precise dosing without requiring complicated calculations or tiny, difficult-to-measure volumes.
With 2mg vials, 2ml of water creates a 1mg/ml concentration. Each 0.1ml contains 100mcg—perfect for peptides dosed in the 100-300mcg range. For 10mg vials, 2ml yields a 5mg/ml concentration suitable for compounds requiring higher doses.
These standardized ratios eliminate dosing confusion. You can quickly calculate your required injection volume using simple math that minimizes errors.
Practical Storage Considerations
The 2ml volume fits perfectly in standard peptide vials. Smaller volumes leave excessive headspace that accelerates degradation, while larger volumes require bigger vials that increase costs and storage space.
Additionally, 2ml provides sufficient solution for multiple doses without creating massive quantities that expire before use. Even at conservative daily doses, most users consume reconstituted peptides within the 28-day bacteriostatic window.
Syringe Compatibility
Standard insulin syringes—the preferred tool for peptide injection—measure volumes up to 1ml (100 units). When you reconstitute with Water for injections 2ml you’ll never need to draw the entire vial content in one syringe.
This compatibility ensures you always use appropriately-sized syringes that provide accurate measurement markings. Trying to draw from overly diluted solutions (reconstituted with 5ml or more) often requires multiple syringe fills, increasing contamination risks and injection complexity.
How to Properly Reconstitute Peptides With Water for Injections 2ml
Mastering reconstitution technique ensures maximum peptide potency while preventing contamination. Follow these steps precisely for optimal results.
Preparation and Sterilization
Before beginning, gather all necessary supplies. You’ll need your peptide vial, bacteriostatic water for injections 2ml, alcohol swabs, and appropriate syringes.
Wash your hands thoroughly with antibacterial soap. Even though you’ll wear gloves, starting with clean hands reduces contamination risks. Consider wearing nitrile gloves throughout the process for additional protection.
Clean your workspace with antibacterial cleaner. A clear, uncluttered surface prevents accidental contamination from environmental sources. Many users perform reconstitution in their kitchen or bathroom, both easily sanitized.
Drawing the Water
Remove the plastic cap from your bacteriostatic water vial, revealing the rubber stopper underneath. Swab the stopper thoroughly with an alcohol pad and allow it to air dry for 30 seconds. Rushing this step by injecting before the alcohol evaporates can introduce isopropyl alcohol into your solution.
Take a 3ml syringe (or two 1ml insulin syringes if needed) and attach a needle. Draw back the plunger to the 2ml mark, filling the barrel with air. This air will replace the water you remove, preventing vacuum formation in the vial.
Insert the needle through the rubber stopper into the
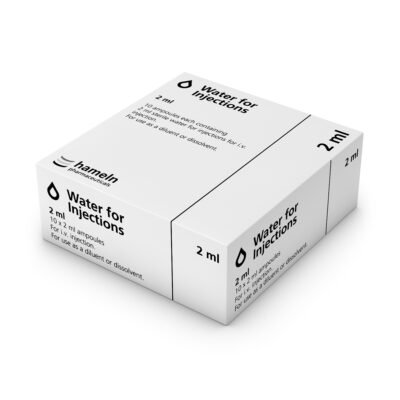
. Push the plunger slowly, injecting the air into the vial. Then invert the vial and slowly draw back the plunger, extracting exactly 2ml of water.
Remove any air bubbles by tapping the syringe barrel and pushing the plunger slightly until only liquid remains. Accurate measurement matters—too little water creates overly concentrated solutions, while excess water unnecessarily dilutes your peptide.
Adding Water to the Peptide Vial
Prepare your peptide vial using the same sterilization process. Remove the cap, swab the stopper with alcohol, and allow it to dry completely.
Here’s where technique becomes critical. Never inject water directly onto the lyophilized powder. The force of impact can damage delicate peptide chains, reducing potency.
Instead, insert your needle and angle it so the water runs down the inside wall of the vial. Inject slowly and steadily, allowing the water to gently contact the powder. The reconstitution should take 15-30 seconds for 2ml.
Some users inject half the water, wait a moment, then add the remainder. This two-stage approach further reduces turbulence that might damage peptides.
Dissolving the Peptide
After adding all the water, resist the urge to shake the vial vigorously. Aggressive agitation damages peptide structures, especially complex proteins like growth hormone.
Instead, gently swirl the vial in circular motions. Allow time for the powder to dissolve naturally—this process might take 1-5 minutes depending on the compound. Some peptides dissolve almost instantly, while others require patient waiting.
If powder remains after several minutes of gentle swirling, you can roll the vial between your palms. The warmth from your hands slightly accelerates dissolution without harmful mechanical stress.
The final solution should appear clear and colorless for most peptides. Cloudiness, color changes, or visible particles indicate contamination or degradation—discard such solutions immediately.
Post-Reconstitution Handling
Once fully dissolved, immediately refrigerate your reconstituted peptide. Most compounds remain stable at room temperature only briefly, degrading rapidly without refrigeration.
Label the vial with the reconstitution date. Bacteriostatic water preserves sterility for 28 days, but many peptides lose potency faster. Knowing exactly when you reconstituted helps you track whether your solution remains viable.
Store the vial upright in your refrigerator, away from the freezer compartment. Freezing reconstituted peptides damages their molecular structure. The main refrigerator compartment (2-8°C) provides ideal storage conditions.
Critical Storage Guidelines for Water for Injections 2ml
Proper storage protects your investment and ensures safety. Both unreconstituted water and reconstituted peptides require specific conditions.
Storing Unopened Water for Injections
Sealed bacteriostatic water vials remain stable for years when stored properly. Keep them at room temperature away from direct sunlight and extreme heat.
Avoid storing water vials in bathrooms despite the convenience. Humidity fluctuations and temperature changes can compromise seal integrity over time. A bedroom drawer or kitchen cabinet away from the stove works better.
Check expiration dates before use. While water doesn’t “spoil” in the traditional sense, the sterility guarantee and bacteriostatic effectiveness have defined limits. Most manufacturers guarantee 2-3 years from production date.
Storing Opened Bacteriostatic Water
After first use, bacteriostatic water remains safe for 28 days when refrigerated. The benzyl alcohol preservative prevents bacterial growth during this window.
However, many users prefer using opened vials within 2 weeks for maximum safety. While the 28-day guideline reflects conservative official recommendations, shorter timeframes provide additional security margins.
Always refrigerate opened bacteriostatic water between uses. Room temperature storage accelerates preservative degradation and increases contamination risks.
Replace the plastic cap after each use to minimize airborne contaminant exposure. While the rubber stopper provides the primary seal, the outer cap offers additional protection.
Storing Reconstituted Peptides
Once you’ve mixed peptides with water for injections 2ml, storage requirements become more stringent. Different peptides have varying stability profiles, but general guidelines apply broadly.
Refrigerate all reconstituted peptides immediately. The 2-8°C temperature range significantly extends peptide half-life compared to room temperature storage.
Most peptides remain potent for 2-4 weeks when refrigerated after reconstitution. However, some compounds degrade faster. Growth hormone, for example, maintains full potency for about 14 days refrigerated, while some shorter peptides remain stable for a month.
Never freeze reconstituted peptides. Ice crystal formation disrupts peptide chains, destroying biological activity. If you accidentally freeze a reconstituted vial, discard it rather than risk injecting damaged compounds.
Protect reconstituted vials from light exposure. Some peptides undergo photodegradation when exposed to UV light. Storing vials in their original boxes or wrapping them in aluminum foil provides protection.
Common Mistakes to Avoid
Understanding frequent errors helps you sidestep problems that plague less experienced users.
Using Inappropriate Water Types
Never substitute regular water, distilled water, or saline for pharmaceutical-grade water for injections. These alternatives contain contaminants or additives that compromise safety when injected.
Tap water contains bacteria, minerals, chlorine, and other substances that trigger immune reactions or infections when injected subcutaneously. Even boiled tap water remains unsuitable due to dissolved solids and potential endotoxins.
Distilled water from grocery stores, while purer than tap water, doesn’t meet pharmaceutical standards. It may contain bacterial contamination and lacks bacteriostatic preservation. Using it means your reconstituted peptides expire within 24 hours.
Saline solution (0.9% sodium chloride) technically works for reconstitution, but it’s not ideal. Some peptides interact poorly with sodium chloride, and saline provides no advantages over proper bacteriostatic water.
Improper Injection Technique During Reconstitution
Forcefully injecting water directly onto lyophilized powder represents the most common reconstitution error. This aggressive technique creates turbulence that damages delicate peptide structures.
The resulting mechanical stress breaks peptide bonds, reducing potency sometimes by 20-30%. You’re essentially destroying a portion of your expensive compounds through careless technique.
Always inject water down the vial’s interior wall, allowing it to gently flow over the powder. This method preserves maximum potency while still achieving complete dissolution.
Shaking Instead of Swirling
Similarly, vigorous shaking damages peptides through mechanical stress. The violent motion slams peptide molecules against the vial walls and creates foam that denatures proteins.
Gentle swirling achieves dissolution without these destructive forces. Patience during this step protects your investment and ensures you receive full potency from each injection.
Neglecting Sterilization Protocols
Failing to swab rubber stoppers with alcohol before each needle insertion invites contamination. Even tiny bacterial loads multiply rapidly in reconstituted solutions.
Additionally, reusing needles or syringes introduces bacteria while dulling the needle point. Always use fresh, sterile needles for both reconstitution and injection.
Incorrect Storage Temperatures
Leaving reconstituted peptides at room temperature accelerates degradation dramatically. Some compounds lose 50% potency within hours at room temperature but remain stable for weeks refrigerated.
Conversely, freezing destroys most peptides completely. The expansion of ice crystals physically tears apart peptide chains. A frozen peptide vial represents a total loss.
Ignoring Expiration Timeframes
Continuing to use bacteriostatic water beyond 28 days after opening risks infection from bacterial growth. Similarly, using peptides weeks after their expected degradation point wastes money on ineffective injections.
Track dates meticulously. Label both your water vials and reconstituted peptides with opening/reconstitution dates. When in doubt, discard questionable solutions rather than risk complications.
Calculating Precise Doses After Reconstitution
Accurate dosing requires understanding the mathematics of reconstitution. Fortunately, the 2ml standard simplifies calculations significantly.
Basic Calculation Formula
The fundamental formula for any reconstituted solution is:
Concentration (mg/ml) = Total Peptide Amount (mg) ÷ Water Volume (ml)
For example, if you reconstitute a 5mg peptide vial with 2ml water: 5mg ÷ 2ml = 2.5mg/ml concentration
This means each 1ml of your solution contains 2.5mg of peptide.
Converting to Micrograms
Most peptide doses use microgram (mcg) measurements. Since 1mg = 1000mcg, multiply your mg/ml concentration by 1000 to get mcg/ml.
Using our previous example: 2.5mg/ml × 1000 = 2500mcg/ml
Now you know each 1ml contains 2500mcg of peptide.
Determining Injection Volume
To calculate how much to inject for your desired dose, divide your target dose by the concentration:
Injection Volume (ml) = Desired Dose (mcg) ÷ Concentration (mcg/ml)
If you want 250mcg from our 2500mcg/ml solution: 250mcg ÷ 2500mcg/ml = 0.1ml
You would inject 0.1ml (10 units on an insulin syringe) to receive 250mcg.
Using Insulin Syringe Markings
Insulin syringes display “units” rather than milliliters. Fortunately, the conversion is straightforward:
- 100 units = 1ml
- 50 units = 0.5ml
- 10 units = 0.1ml
Therefore, in our example, you would draw to the 10-unit mark on your insulin syringe to inject 250mcg.
Creating a Dosing Chart
For convenience, create a reference chart after reconstituting each vial. List common doses alongside their corresponding syringe units.
Example for 5mg in 2ml (2500mcg/ml concentration):
- 100mcg = 4 units
- 200mcg = 8 units
- 250mcg = 10 units
- 500mcg = 20 units
This chart eliminates mental math before each injection, reducing errors when you’re rushed or tired.
Safety Protocols and Contamination Prevention
Maintaining sterility throughout the reconstitution and administration process protects your health while preserving peptide integrity.
Hand Hygiene and Workspace Preparation
Always begin by washing hands thoroughly with antibacterial soap for at least 20 seconds. Pay attention to areas between fingers and under nails where bacteria concentrate.
Dry hands with clean paper towels rather than cloth towels that might harbor bacteria. Consider using hand sanitizer as an additional precaution after washing.
Prepare your workspace by wiping surfaces with alcohol-based cleaner or diluted bleach solution. Allow the surface to air dry completely before placing supplies.
Gather all materials before starting. Having everything within reach prevents interruptions that increase contamination risks.
Proper Alcohol Swabbing Technique
Use fresh alcohol swabs for each rubber stopper puncture. A single swab used multiple times becomes contaminated and ineffective.
Swab in circular motions from the center outward, covering the entire rubber surface. Apply moderate pressure to ensure the alcohol penetrates any microscopic cracks or crevices.
Most importantly, allow alcohol to air dry for 30 seconds before inserting your needle. Wet alcohol doesn’t sterilize effectively, and injecting alcohol-soaked material into your peptide solution dilutes the bacteriostatic preservative.
Needle and Syringe Management
Never reuse needles or syringes, even for drawing from the same vial. Each use dulls the needle point and introduces contamination.
When preparing multiple injections, use separate syringes for each. Cross-contamination between doses or vials can introduce bacteria or mix incompatible compounds.
Never touch the needle or allow it to contact non-sterile surfaces. If the needle touches anything except the rubber stopper, discard it and use a fresh one.
Recognizing Contamination Signs
Learn to identify contaminated solutions before injecting them. Clear solutions that become cloudy indicate bacterial growth or chemical degradation.
Visible particles, floating debris, or color changes all signal problems. Discard any solution that doesn’t appear crystal clear (for peptides that reconstitute to clear solutions).
Unusual odors when opening vials suggest bacterial contamination. While most peptides have minimal scent, strong chemical or organic smells indicate problems.
If you develop persistent injection site reactions—redness, swelling, pain lasting beyond 24 hours—suspect contamination. Discontinue use of that vial and consult a healthcare provider if symptoms worsen.
Medical Applications vs. Performance Enhancement Uses
Water for injections 2ml serves diverse purposes across medical and performance enhancement contexts. Understanding these applications provides broader perspective.
Legitimate Medical Applications
Healthcare providers use WFI for reconstituting numerous medications. Antibiotics, vaccines, chemotherapy agents, and hormone replacement therapies all require pharmaceutical-grade water.
Diabetes patients use bacteriostatic water when reconstituting certain insulin formulations. Fertility treatments involving injectable hormones rely on proper WFI usage.
Medical settings follow strict protocols for reconstitution, storage, and administration. These standards ensure patient safety while maximizing medication effectiveness.
Performance Enhancement and Anti-Aging
Athletes and bodybuilders use water for injections 2ml primarily for reconstituting peptides and growth hormone. These compounds enhance muscle growth, accelerate fat loss, and improve recovery.
Anti-aging clinics utilize WFI for hormone optimization protocols. Patients receive various peptides, growth factors, and hormones reconstituted with pharmaceutical-grade water.
While these applications occur outside traditional medical supervision, the same safety principles apply. Proper technique, sterile handling, and appropriate storage remain essential regardless of usage context.
Research and Development
Scientists employ water for injections when preparing experimental compounds for laboratory research. The pharmaceutical-grade purity ensures research accuracy by eliminating confounding variables.
This research application explains why many online vendors market products “for research purposes only”—a legal disclaimer distancing them from human consumption implications.
Purchasing Genuine Water for Injections 2ml
Obtaining legitimate pharmaceutical-grade water ensures safety and effectiveness. The market contains various quality levels requiring careful navigation.
Identifying Reputable Suppliers
Look for vendors specializing in research chemicals or pharmaceutical supplies. Companies serving medical professionals and laboratories typically maintain higher quality standards than general retailers.
Check for third-party testing certificates. Legitimate suppliers test their water for sterility, endotoxins, and pH levels. They willingly provide documentation proving their products meet pharmaceutical standards.
Read customer reviews carefully, looking for detailed feedback from experienced users. Generic praise means little, but specific comments about product quality and supplier reliability provide valuable insights.
Price Considerations
Extremely cheap water for injections should raise concerns about quality or authenticity. Pharmaceutical-grade production involves costs that establish realistic minimum pricing.
Conversely, exorbitant prices don’t guarantee superior quality. Some vendors exploit uninformed consumers by dramatically marking up standard products.
Expect to pay $3-8 per 2ml vial depending on quantity purchased. Bulk orders typically reduce per-unit costs while ensuring you always have supplies available.
Packaging and Labeling
Legitimate pharmaceutical water arrives in properly sealed vials or ampoules with professional labeling. The packaging should include:
- Production date
- Expiration date
- Lot number
- Ingredients (sterile water or bacteriostatic water with 0.9% benzyl alcohol)
- Manufacturer information
- Storage instructions
Poor quality printing, spelling errors, or missing information suggests counterfeit or substandard products.
Storage Capacity Planning
Calculate your needs based on usage patterns. If you regularly use peptides, maintaining a 6-12 month supply of water for injections makes sense.
Sealed bacteriostatic water remains stable for years when properly stored. Buying larger quantities reduces per-unit costs while ensuring you never run out mid-cycle.
However, avoid excessive hoarding. While sealed vials last indefinitely, quality can degrade over extremely long periods. Purchase amounts you’ll reasonably use within 2-3 years.
Regulatory Standards and Pharmaceutical Grade Classifications
Understanding the regulatory framework behind water for injections provides confidence in product selection and usage.
USP Standards
In the United States, the U.S. Pharmacopeia (USP) establishes standards for pharmaceutical products including Water for injections 2ml. USP-grade water meets specific purity requirements for:
- Total dissolved solids (maximum 10 ppm)
- Bacterial endotoxins (less than 0.25 EU/ml)
- Bacterial counts (zero viable organisms)
- pH levels (5.0-7.0)
Products labeled “USP grade” have undergone testing confirming compliance with these rigorous standards.
European Pharmacopoeia Standards
The European Pharmacopoeia (Ph. Eur.) establishes similar standards for European markets. These specifications align closely with USP requirements while incorporating some regional variations.
Products meeting Ph. Eur. standards provide equivalent quality and safety to USP-grade water. Many international suppliers reference both standards in their documentation.
Good Manufacturing Practice (GMP) Certification
Facilities producing pharmaceutical-grade water should operate under Good Manufacturing Practice guidelines. GMP certification ensures consistent quality control, proper contamination prevention, and reliable production processes.
When evaluating suppliers, preference goes to those manufacturing in GMP-certified facilities. This certification indicates serious commitment to quality rather than profit-driven corner-cutting.
Sterility Testing Methods
Manufacturers employ various testing methods to verify sterility. These include:
- Direct inoculation testing (introducing samples into culture media)
- Membrane filtration (filtering samples to capture any organisms)
- Rapid microbiological methods (using technology to detect contamination quickly)
Reputable suppliers perform batch testing and maintain certificates of analysis (COAs) proving sterility for each production lot.
Environmental and Disposal Considerations
Responsible usage extends beyond personal safety to environmental stewardship and proper waste management.
Proper Disposal of Used Water Vials
Empty Water for injections 2ml vials should go into sharps containers along with used needles and syringes. While the vials themselves aren’t sharp, consolidating all medical waste simplifies disposal.
Many communities offer sharps disposal programs through pharmacies, hospitals, or waste management services. Never discard sharps containers in regular trash where they might injure sanitation workers.
Some areas allow home disposal of sealed sharps containers in regular trash after filling them only 3/4 full and securing lids with heavy tape. However, check local regulations, as requirements vary significantly.
Medication Waste Considerations
Never pour unused reconstituted peptides down drains or toilets. Pharmaceutical compounds entering Water for injections 2ml supplies create environmental problems and affect aquatic ecosystems.
Instead, mix unused solutions with undesirable substances like coffee grounds or cat litter in sealed bags before trash disposal. This prevents accidental consumption by children or animals.
Some pharmacies operate medication take-back programs accepting unused pharmaceuticals for proper disposal. These programs ensure environmental safety while preventing medication diversion.
Reducing Waste Through Planning
Minimize waste by carefully planning your peptide purchases and reconstitution timing. Only reconstitute amounts you’ll use within stability windows.
Purchase peptides in vial sizes matching your dosing protocols. Using a 10mg vial when you only need 2mg creates unnecessary waste when the reconstituted solution expires before complete usage.
Similarly, avoid buying excessive quantities of water for injections beyond what you’ll reasonably use. While properly stored vials last years, eventual expiration means even water can become waste.
Frequently Asked Questions About Water for Injections 2ml
Addressing common questions helps clarify remaining uncertainties about this essential product.
Can I reuse bacteriostatic water after 28 days?
While technically possible, doing so increases infection risks significantly. The benzyl alcohol preservative loses effectiveness over time, and bacterial contamination becomes increasingly likely.
The cost of replacement water seems minimal compared to potential health consequences from infected injections. Always prioritize safety over minor cost savings.
What happens if I accidentally freeze my water for injections?
Freezing water for injections doesn’t damage the water itself. Unlike peptides, simple water tolerates freezing and thawing without structural damage.
However, freezing can compromise container integrity. Glass vials might crack from expansion, and rubber stoppers might loosen, breaking sterility seals.
If you accidentally freeze sealed Water for injections 2ml, inspect them carefully after thawing. Discard any with visible cracks or compromised seals. Intact vials remain safe for use.
Can I use water for injections for intramuscular injections?
Yes, water for injections works for both subcutaneous and intramuscular administration. The pharmaceutical-grade purity makes it safe for anyWater for injections 2ml route.
However, most peptides and growth hormone protocols specify subcutaneous injection. Follow your specific compound’s administration guidelines rather than assumingWater for injections 2ml routes.
How do I know if my water for injections has gone bad?
Properly stored, sealed Water for injections 2ml remains viable essentially indefinitely. However, signs of contamination or degradation include:
- Cloudiness or particulate matter
- Unusual odors when opening the vial
- Discolored water (should be completely clear)
- Compromised seals or damaged vials
- Expiration date passage
When doubt exists, discard questionable vials rather than risk complications.
Is tap water safe if I filter it really well?
No amount of home filtration achieves pharmaceutical-grade purity. Even advanced reverse osmosis systems leave trace contaminants and cannot guarantee sterility.
Additionally, filtered water lacks bacteriostatic preservation, making reconstituted peptides unsafe within 24 hours. The minimal cost of proper water for injections makes homemade alternatives unnecessarily risky.
Be the first to review “Water for injections 2ml x 10amps” Cancel reply
Related products
Syringes & Accessories
Anavar - Oxandrolone
Syringes & Accessories
Syringes & Accessories
Syringes & Accessories
Drawing Needles
Syringes & Accessories
Syringes & Accessories








Reviews
There are no reviews yet.